CRANIAL NERVE PALSY FAQ
FAQ
Cranial nerves are parts of the peripheral nervous system that supply the muscles of eye movement. Cranial nerve 3 supplies majority of the extraocular muscles, while cranial nerve 4 and 6 supplies the superior oblique and the lateral rectus, respectively.
A weakness in the power of the particular nerve would lead to an inability of the muscle or muscles to move the eyeball in a particular position. This imbalance in the forces of eye movement produces particular eye movement abnormalities that help the pediatric ophthalmologist in making the clinical diagnosis.
Congenital cranial nerve palsies usually present with a compensatory face turn, head tilt or chin-up position.
The acquired form is usually accompanied by complaints of diplopia or double vision. Overall, the common etiologies in children and adolescents include the following, in decreasing order: neoplasm (tumor), idiopathic, inflammation, and non-aneurysmal vascular problem. Neoplasm is the most common cause of cranial nerve 6 and cranial nerve 3 palsies, while the decompensated congenital form is the the most common cause of acquired cranial nerve 4 palsy in children and adolescents.
The etiology of the acquired form in adults include aneurysms, trauma, and infection.
The pediatric ophthalmologist could order a neuroimaging test (like MRI) and limited blood works for those patients with microvascular risk factors.
The indications for treatment are the same reasons that brought patients to seek consultation: diplopia and abnormal head turn.
For the acutely presenting acquired form, botulinum toxin A (Botox) can be injected into the antagonist muscle to prevent contracture, while waiting for the paretic muscle to recover, which could take up to 6 months. The effect of Botox injection is noticeable within 2 weeks and could last up to 4 months. It is ideal to do the injection within one month of the onset of symptom, before contracture of the antagonist sets in. Within 2 months of observation, the pediatric ophthalmologist would have an idea whether the paretic muscle is recovering.
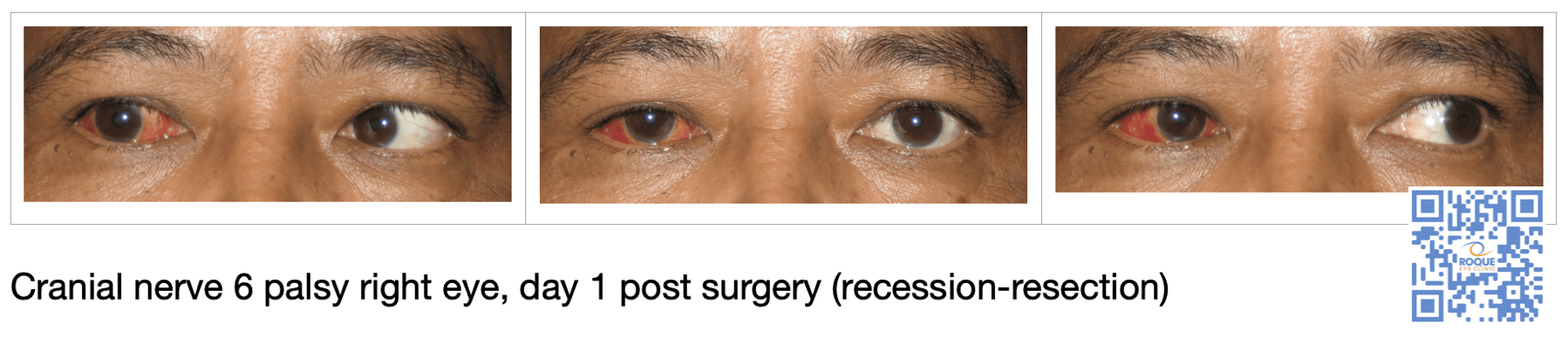
A residual eye deviation requires surgical intervention to improve eye movement and lateral incomitance. Surgery on the involved eye muscle or muscles can be in the form of recession-resection, or transposition, or muscle split, or a combination, depending on the complexity of the eye deviation. There is a potential for a second surgery when several muscles are involved.
- Basiakos, S., Graf, M., Preising, M., and Lorenz, B. (2019). Splitting of the lateral rectus muscle with medial transposition to treat oculomotor palsy: a retrospective analysis of 29 consecutive cases. Graefes Arch Clin Exp Ophthalmol, 257(9): 2005-2014.
- Escuder, A. and Hunter, D. (2019). The role of botulinum toxin in the treatment of strabismus. Semin Ophthalmol, 34(4): 198-204.
- Park, K., Oh, S., Min, J., Kim, B., and Kim, Y. (2019). Acquired onset of third, fourth, and sixth nerve palsies in children and adolescents. Eye (Lond), 33(6): 965-973.
- Pineles, S., and Velez, F. (2018). Isolated ocular motor nerve palsies. J Binol Vis Ocul Motil, 68(3): 70-77.
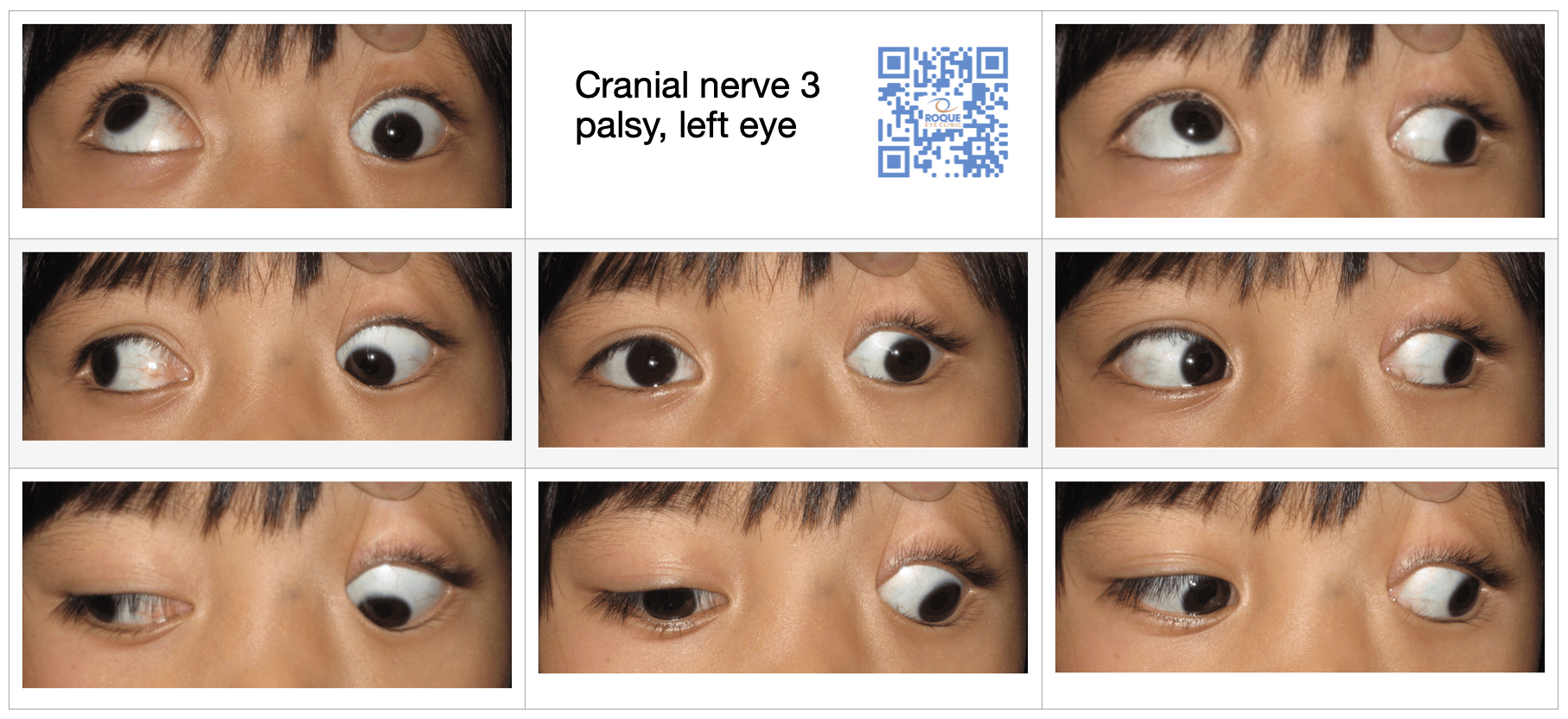
CN 3 PALSY

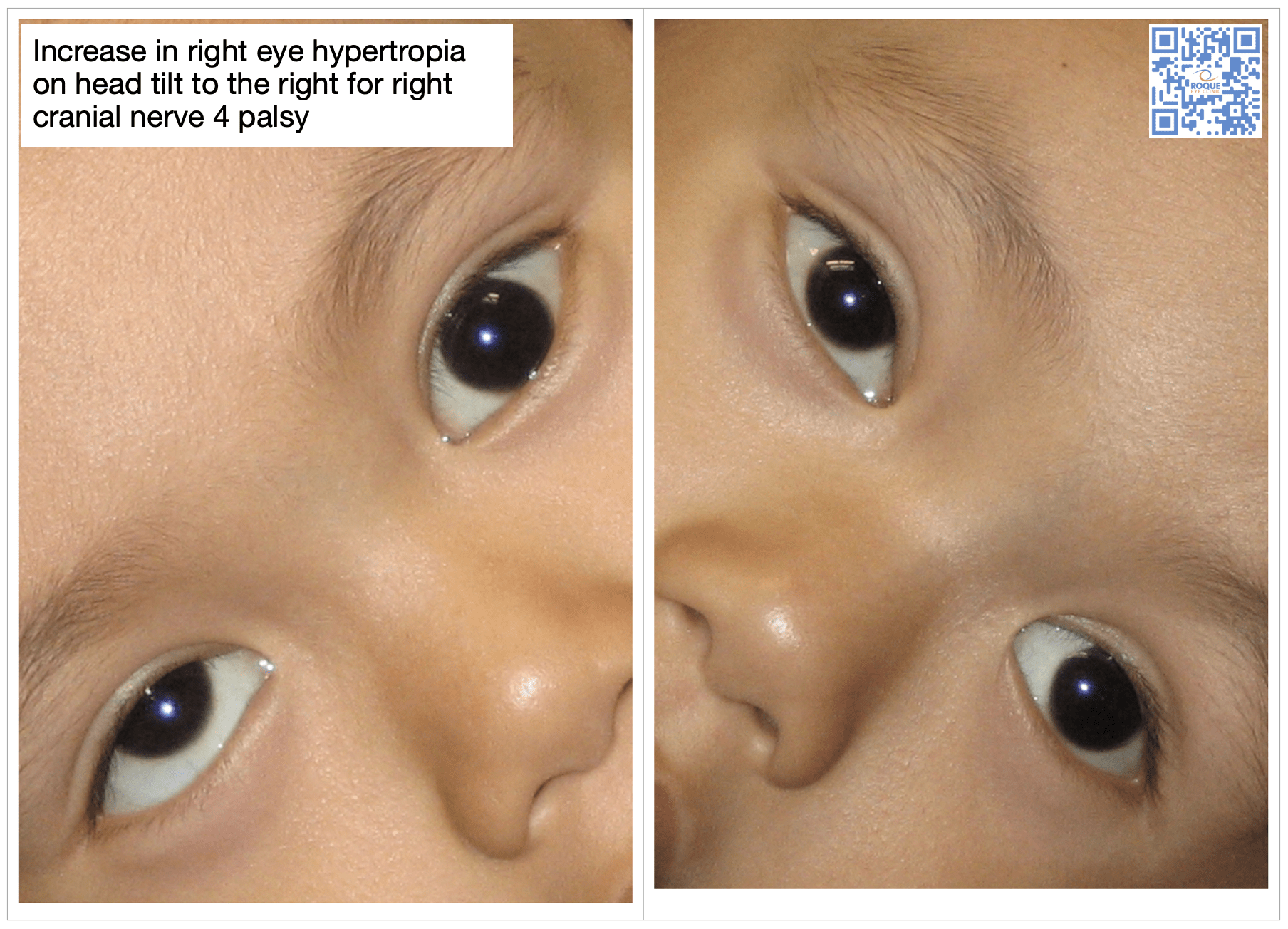
CN 4 PALSY
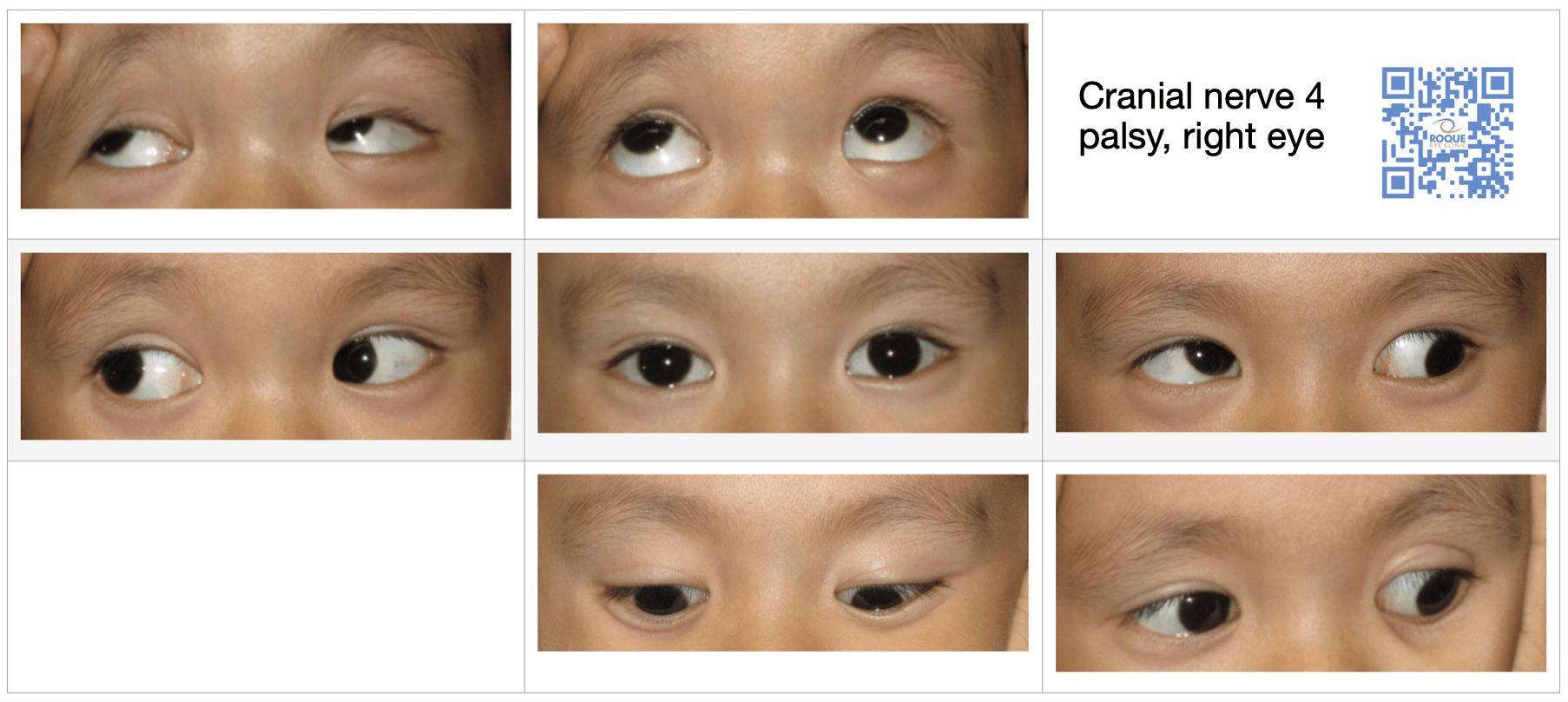
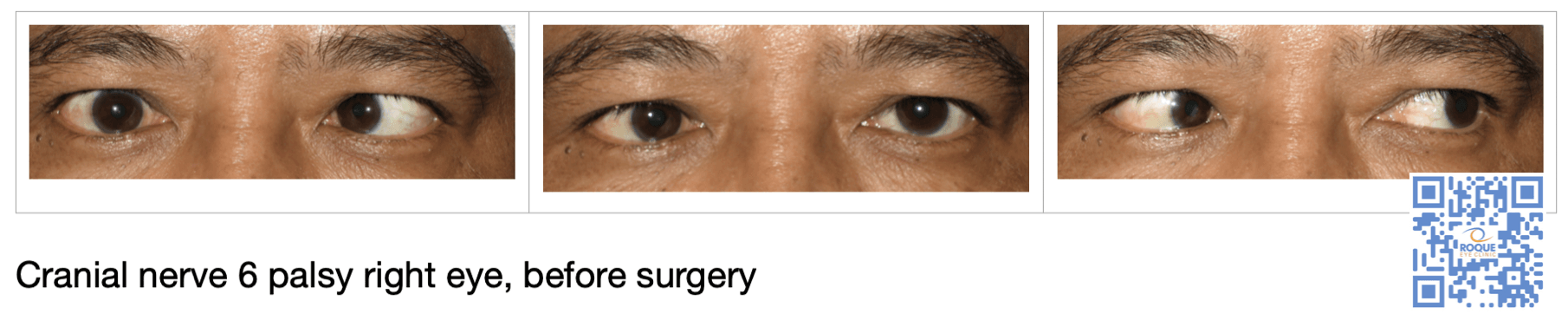
CN 6 PALSY
BOOK AN APPOINTMENT
It takes less than 5 minutes to complete your online booking. Alternatively, you may call our BGC Clinic, or our Alabang Clinic for assistance.
OUR SPECIALIST
DR. BARBARA ROQUE
MD, DPBO, FPAO, FPCS
Dr. Barbara Roque is a specialist in pediatric ophthalmology, adult strabismus, and ophthalmic genetics. Her private practice began in 2006, after her post-graduate fellowship training at The Children’s Hospital in Westmead, University of Sydney System, Australia. Her patients are mostly children with ocular disease, refractive errors, cataracts, and eye misalignment.
OUR CLINICS
BGC CLINIC
- ST. LUKE'S MEDICAL CENTER GLOBAL CITY
2/F Medical Arts Building 217
Rizal Drive corner 5th Avenue
Bonifacio Global City, Taguig 1634
Philippines
SLMC CLINIC HOURS
- 9am - 12pm
Appointments only
ALABANG CLINIC
- ASIAN HOSPITAL AND MEDICAL CENTER
5/F Medical Office Building 509
2205 Civic Drive, Filinvest City
Alabang, Muntinlupa 1781
Philippines
AHMC CLINIC HOURS
- 1pm - 4pm
Appointments only
BOOK AN APPOINTMENT
It takes less than 5 minutes to complete your online booking. Alternatively, you may call our BGC Clinic, or our Alabang Clinic for assistance.