Retina and Vitreous: Symptoms, Diseases, and When You Need Urgent Eye Care
A patient-friendly guide to the back of the eye, including floaters, flashes, diabetic retinal disease, macular disease, retinal tears, retinal detachment, bleeding, and when delay can threaten vision.
🧠 Dr. Roque’s Quick Answer
The retina is the light-sensitive tissue at the back of the eye, and the vitreous is the clear gel that fills the inside of the eye. Problems in this area can cause floaters, flashes, blurred vision, distortion, bleeding, or sudden vision loss. Some are chronic and manageable. Others, such as a retinal tear or retinal detachment, may need urgent treatment to protect sight.
🎯 Focus
Explain what the retina and vitreous do and why disease in this area can threaten vision.
🏁 Goal
Help patients recognize warning signs, understand common diagnoses, and know the next safe step.
🛡️ Evidence-Based
Retina and vitreous disorders range from gradual diseases to true emergencies such as retinal tears and retinal detachment.
🧠 Dr. Roque’s Key Learning Points
- The retina handles vision signals. The vitreous is the gel inside the eye.
- New floaters and flashes deserve attention because they can signal vitreous change, a retinal tear, or retinal detachment.
- Distorted central vision can point to macular disease.
- Diabetes can damage the retina even before vision changes become obvious.
- Sudden shadow, curtain, major drop in vision, or new shower of floaters should be treated as urgent.
Quick Navigation
ROQUE Eye Clinic Retina and Vitreous Knowledge Hub
This page serves as a cornerstone overview for retina and vitreous disease.
You can also start from the main conditions hub: Conditions
👁️ Anatomy Micro-Primer
- Retina: the light-sensitive tissue lining the back of the eye.
- Macula: the central part of the retina responsible for sharp straight-ahead vision.
- Peripheral retina: the outer retina that helps with side vision and motion awareness.
- Vitreous: the clear gel that fills the center of the eye and lies against the retina.
- Retinal blood vessels: supply oxygen and nutrients to retinal tissue.
🧩 Terminology Glossary
- Floaters: moving spots, threads, or cobweb-like shadows in vision.
- Flashes: brief light streaks or flickers, often from vitreous traction on the retina.
- Posterior vitreous detachment: a common age-related separation of the vitreous from the retina.
- Retinal tear: a break in the retina that may lead to detachment.
- Retinal detachment: separation of the retina from the tissue beneath it.
- Macular degeneration: disease affecting the macula and central vision.
- Diabetic retinopathy: diabetes-related damage to retinal blood vessels.
- Vitreous hemorrhage: bleeding into the vitreous gel.
What Are the Retina and Vitreous?
The retina works like the eye’s camera sensor. It captures light and converts it into signals that travel to the brain. The vitreous is the clear gel filling the inside of the eye. It helps the eye keep its shape and sits next to the retina.
This matters because many symptoms that patients describe as “blurred vision,” “floaters,” “dark spots,” “distortion,” or “a curtain in the vision” can come from disease in the retina or vitreous.
💡 Dr. Roque’s Analogy
Think of the retina as the film or sensor at the back of a camera, and the vitreous as the clear jelly inside the camera body. If the sensor is damaged, vision quality drops. If the jelly pulls, bleeds, or clouds up, the image can become distorted, blocked, or suddenly dark.
Common Symptoms of Retina and Vitreous Problems
- new floaters
- light flashes
- blurred vision
- distorted or wavy central vision
- a dark curtain, veil, or shadow
- missing part of the visual field
- difficulty reading or recognizing faces
- sudden drop in vision
- blood-like haze or smoky vision
Here is the mistake to avoid: many retina diseases are not painful. Patients often expect severe eye pain if something serious is happening. That assumption is wrong. Some sight-threatening retinal conditions cause little or no pain at all.
Common Retina and Vitreous Conditions
Posterior Vitreous Detachment
As we age, the vitreous can shrink and separate from the retina. This is called a posterior vitreous detachment. Many cases are not dangerous by themselves, but the process can sometimes pull hard enough to create a retinal tear. That is why new floaters and flashes should not be dismissed casually.
Retinal Tear
A retinal tear is a break in the retina. It may start with sudden floaters, flashes, or a change in peripheral vision. A tear can allow fluid to pass under the retina and lead to retinal detachment.
Retinal Detachment
Retinal detachment is more urgent. Patients may describe a curtain, veil, shadow, or sudden missing area in the vision. Vision can fall quickly, especially if the central retina becomes involved. This is not something to “watch for a few weeks.”
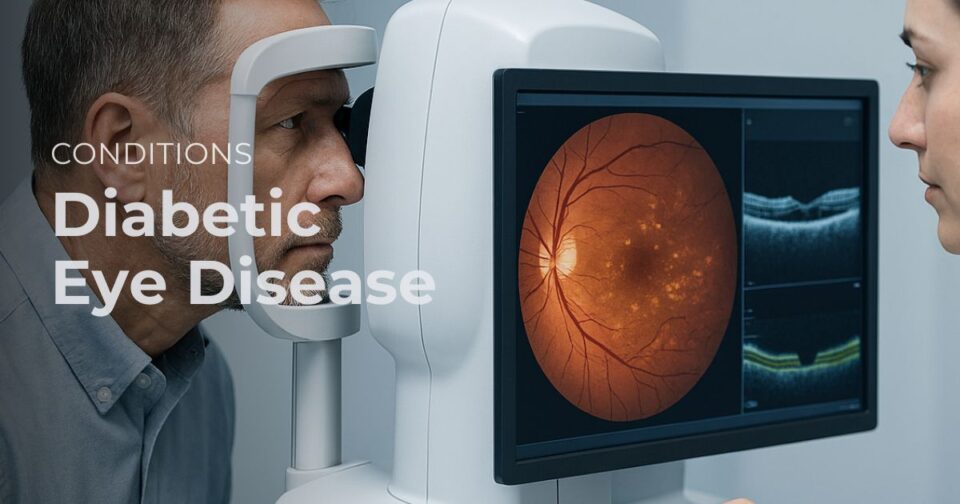
Diabetic Retinopathy and Diabetic Macular Edema
Diabetes can damage retinal blood vessels. Early diabetic retinopathy may cause no symptoms, which is exactly why waiting for symptoms is a weak strategy. As the disease worsens, bleeding, swelling, scarring, and retinal complications may develop. If fluid collects in the macula, central vision may blur.
Age-Related Macular Degeneration
Macular degeneration affects central vision. Patients may notice distortion, waviness of straight lines, difficulty reading, faded detail, or a blur in the center of vision. This is different from a retinal tear or detachment, but it is still a retina problem that deserves proper monitoring and treatment planning.
Vitreous Hemorrhage
Bleeding into the vitreous can cause a shower of floaters, smoky vision, or a sudden darkening of sight. Common causes include diabetic retinal disease, retinal tears, and other vascular retinal conditions. The key point is simple: sudden blood-like haze in vision is not normal.
Retinal Vein or Artery Problems
Blockage of retinal vessels can reduce vision suddenly or subacutely. Some cases affect central vision, while others can damage the broader retina. These often need prompt evaluation because they may also reflect general vascular risk.
Macular Hole, Epiretinal Membrane, and Other Macular Disorders
These conditions often cause distortion, difficulty reading, or reduced central sharpness. Patients may notice that straight lines look bent or that one eye sees less clearly than the other.
When Retina or Vitreous Symptoms May Be an Emergency
🚨 Dr. Roque’s Emergency Warning
Seek urgent eye care if you develop any of the following:
- sudden new floaters, especially many at once
- flashes of light
- a curtain, veil, or shadow over the vision
- sudden major blur or vision loss
- blood-like haze or smoky vision
- sudden distortion of central vision
- vision changes after eye trauma
Do not anchor on a false reassurance like, “It’s probably just stress,” or “It’s only because I’m tired.” That reasoning can cost time you may not safely have.
How Retina and Vitreous Problems Are Diagnosed
Diagnosis starts with the story: what changed, how fast it changed, and whether symptoms involve floaters, flashes, distortion, missing vision, or sudden blur.
The examination may include:
- dilated retinal examination
- careful peripheral retinal assessment
- optical coherence tomography (OCT) for the macula and retina
- retinal imaging or photography when appropriate
- ultrasound in selected cases, especially if bleeding clouds the view
- fluorescein angiography or other vascular testing in some retinal diseases
One weak assumption patients often make is this: “If I can still see, it must not be serious.” That is not bulletproof thinking. Some retinal problems begin before total vision collapse.
Treatment Depends on the Diagnosis
Observation and Monitoring
Some vitreous changes can be monitored if no retinal tear or detachment is found and symptoms remain stable.
Laser or Cryotherapy
Retinal tears are often treated to reduce the risk of progression to detachment.
Intravitreal Injections
Some retinal diseases, especially those involving leakage, swelling, or abnormal blood vessels, may be treated with injections into the eye.
Vitrectomy Surgery
Vitrectomy may be needed in selected cases such as vitreous hemorrhage, retinal detachment, traction, or some macular conditions.
Retinal Detachment Repair
Retinal detachment may require urgent procedural or surgical repair. Timing matters.
Systemic Disease Control
Good diabetes, blood pressure, and vascular risk control matters because the eye is not isolated from the rest of the body.
What Patients Should Not Do
- Do not ignore sudden floaters or flashes.
- Do not assume lack of pain means lack of danger.
- Do not wait weeks if a curtain or shadow develops.
- Do not skip dilated retinal exams if you have diabetes.
- Do not self-diagnose “just aging” without an exam when symptoms are new.
✅ Dr. Roque’s Take-Home Message
Retina and vitreous disease is not one diagnosis. It is a whole group of conditions affecting the back of the eye. Some are chronic and manageable. Some are time-sensitive. The safest mindset is simple: new floaters, flashes, distortion, curtain-like shadow, blood-like haze, or sudden vision loss should not be minimized. Early diagnosis can protect vision.
Frequently Asked Questions
Are floaters always dangerous?
No. Some floaters are benign. But new floaters, especially if paired with flashes or a shadow, need prompt assessment.
What is the difference between a retinal tear and retinal detachment?
A retinal tear is a break in the retina. A detachment means the retina has separated from its underlying support. A tear can lead to detachment.
Can diabetic retinal disease start before I notice symptoms?
Yes. That is why regular eye exams matter even when vision still feels “fine.”
Do retinal problems always cause pain?
No. Many retinal conditions are painless.
What does a macular problem usually feel like?
Patients often describe blur in the center, wavy lines, distorted faces, or trouble reading.
Can a vitreous hemorrhage clear on its own?
Sometimes the blood can settle or clear, but the underlying cause still needs proper evaluation.
Is sudden vision loss from the retina always permanent?
Not always, but delay can worsen the outcome. Speed matters.
If one eye seems normal, can I still have a serious retinal problem in the other eye?
Yes. One eye can compensate, which is why some patients notice the problem late.
Do I need dilation for retina evaluation?
Very often, yes. A dilated exam is commonly needed to assess the retina properly.
When should I book a retina consultation?
Book promptly for new symptoms, known diabetic eye disease, macular distortion, unexplained blur, or any concern about retinal bleeding, tears, or detachment.
📚 Related Reading
📖 References
- National Eye Institute. Retinal Detachment resources.
- National Eye Institute. Diabetic Retinopathy resources.
- American Academy of Ophthalmology. Diabetic Retinopathy Preferred Practice Pattern and retina-related guidance.
- American Academy of Ophthalmology. Preferred Practice Pattern publication schedule and retina benchmarks.
- Authoritative ophthalmology review resources on posterior vitreous detachment, retinal tears, retinal detachment, macular disease, and vitreous hemorrhage.
ROQUE Eye Clinic Patient Education Series
Reviewed by the Roque Advisory Council
Dr. Manolette Roque | Dr. Barbara Roque
St. Luke’s Medical Center Global City | Asian Hospital Medical Center
Philippines
Medical Disclaimer: This page is for patient education only and does not replace an eye examination, diagnosis, or treatment plan. Sudden floaters, flashes, a curtain-like shadow, sudden blur, or sudden vision loss require prompt medical attention.