Age-Related Macular Degeneration
Aging Eye Conditions
Eye disorders are becoming more common with aging. As our aging population grows bigger, awareness of these conditions is extremely important to prevent life altering significant visual loss.
Recent advances in ophthalmology have helped in preventing or correcting eye problems. With early detection and treatment it is still possible for people to maintain good vision as they grow older.
Regular visits to an ophthalmologist (eye specialist) will help in early detection of eye conditions at the time when they can be treated. An ophthalmologist is a medical doctor with special training and skills to diagnose and treat all diseases and disorders of the eye.
Age-Related Macular Degeneration
The macula contains photoreceptors, the light sensitive retinal cells which are responsible for this function. With a normal and healthy macula, activities of daily living such as reading, cross-stitching, driving and recognizing faces are possible.
These activities become increasingly difficult for people afflicted with AMD. With AMD people experience blurring or darkness in the center of their vision and common tasks such as reading and driving are affected. The words on a page may look blurred; a dark or empty area may appear in the center of vision; or straight lines may look distorted. AMD primarily affects central vision but the peripheral vision is usually preserved. For example, you can see the outline of a person but not recognize his or her face.
ANIMATION
2 Forms of AMD
The macula is a metabolically active tissue in the eye. The processes of metabolic waste removal, as well as nutrient and oxygen supply are important in its maintenance. Deficiencies in these processes will lead to macular degeneration.
Dry AMD
Dry AMD is an early stage of the disease and results from the thinning out of photoreceptors in the macula. With aging, yellowish spots known as drusen may begin to accumulate as metabolic waste pile up with the progressive inability of the eye to remove these in the macula. This coupled with decrease in the supply of nutrients and oxygen to the macula leads to losses in its light sensitive retinal cells. Gradual central vision loss may occur with dry AMD.
Wet AMD
In wet AMD, new blood vessels grow (neovascularization) beneath the macula. In an attempt to re-establish oxygenation and nutrient support the body creates new vessels. This is the body's abnormal way of repairing itself. The neovascularization causes leakage of blood and fluid. This leakage causes severe injury to the light-sensitive retinal cells, which die off and create blind spots in central vision. The process creates severe photoreceptor damage and scarring, leading to severe central vision loss.
2 Categories of Neovascularization
Classic CNV
Occult CNV
DIAGNOSIS OF AMD
Upon your visit to your ophthalmologist, he will first check your reading vision (visual acuity). The smaller the letters that you can read, the better is your visual acuity. Contrast sensitivity, the ability to recognize letters of decreasing darkness against a white background, may also be tested. Macular problems such as AMD will present as decreased visual acuity and contrast sensitivity.
The Amsler grid is also a helpful tool in detecting and monitoring macular diseases such as AMD. A test card with lines in a grid pattern with a central dot is used. The test is done using one eye at a time. With the eye fixating at the central dot, the lines are normally straight and complete. With macular problems such as AMD broken lines, wavy lines, or dark shades or spots are observed. Patients with wet AMD and those at risk are advised daily Amsler grid testing with the instructions to consult immediately if changes are noted.
A dilated fundus examination is done to examine the retina. With special lenses your ophthalmologist examines the macula. Lesions such as drusen and areas of atrophy are visualized in dry AMD. With wet AMD, exudation and/or hemorrhaging are present.
A fluorescein angiogram is done to examine the circulation in the macula. A fluorescent dye is injected into the arm and, with the use of a special fundus camera, pictures of the retina are taken serially. The retina is observed while the dye fills the retinal vessels. Wet AMD is observed as abnormal fluorescence developing from leakage of dye in the macula.
Optical coherence tomography (OCT) of the macula is another diagnostic modality which is done to detect fluid/blood and structural changes in the macula. This is useful in monitoring for progression of the disease or response to treatment.
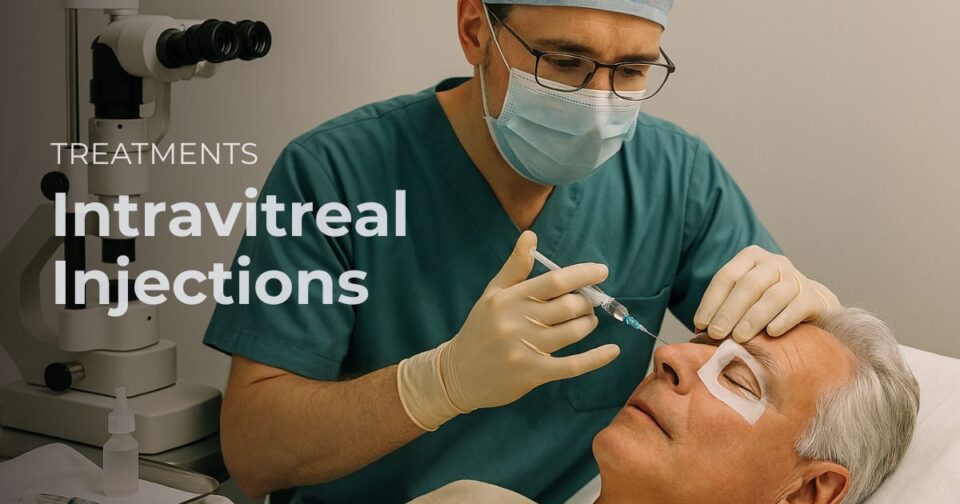
TREATMENT OF AMD
Until recently, ophthalmologists could only offer treatment for wet AMD that reduced the risk of additional vision loss, rarely leading to visual improvement and recovery. In the advanced stage, patients endured inevitable loss of central vision.
The discovery of vascular endothelial growth factor inhibitors (anti-VEGF) has revolutionized the management of wet AMD. Anti-VEGF treatment has been proven in clinical studies to increase the chance of visual improvement and not only reduce the risk of vision loss among patients with wet AMD.
Anti-VEGF medications that have been used to treat wet AMD include Aflibercept (Eylea), Ranibizumab (Lucentis), Pegaptanib (Macugen) and Bevacizumab (Avastin). Eylea, Lucentis and Macugen have received U.S. Food and Drug Administration approval for the treatment of wet AMD. Avastin has been used off-label for wet AMD and is presently being evaluated. These new macular degeneration drugs were celebrated as a major medical breakthrough.
Treatment involves injection of the medication into the affected eye. This is done once every 4 to 6 weeks to maintain the desired effect. Close follow-up is done to monitor treatment response.
Presently there are no US FDA-approved treatments available for dry AMD. A major study (Age-Related Eye Disease Study) has produced evidence that intake of certain nutrients such as vitamins A (beta carotene), C and E may help prevent or slow progression of dry macular degeneration.
It is also recommended that dry AMD patients wear sunglasses with UV protection against potentially harmful effects of the sun. Daily Amsler Grid monitoring is also advised to monitor for development of wet AMD.
ANIMATION
AddOn SML (Scharioth Macula Lens) from 1stQ Deutschland GmbH on Vimeo.
Presentation of the AddOn SML, an Intraocular Lens developed for patients suffering from dry AMD to restore their near vision. Based on proven AddOn Technology by 1stQ Deutschland GmbH & Co. KG, Germany. Interview with the Inventor, Prof. Dr. Dr. Gabór Scharioth, Recklinghausen/Germany.
BOOK AN APPOINTMENT
It takes less than 5 minutes to complete your online booking. Alternatively, you may call our BGC Clinic, or our Alabang Clinic for assistance.